This is how Preston and Chorley A&E is struggling to cope during our long hot summer
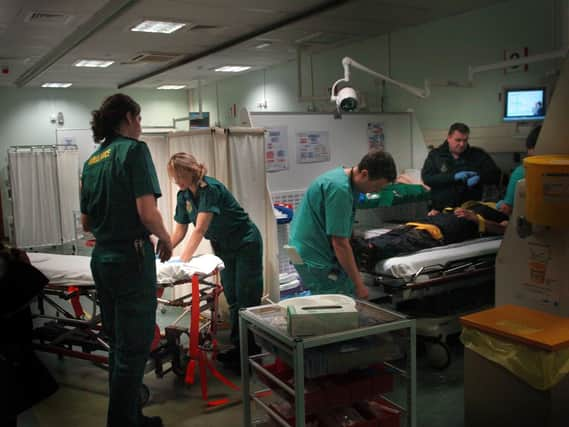

New figures show that hundreds more people attended Preston and Chorley’s A&E departments than this time last year, which health bosses said was an “unprecedented summer surge” due to the heatwave.
The NHS England figures show that 13,487 people attended Lancashire teaching Hospitals Trust’s emergency departments last month, 627 more than in July 2017. Attendances in June were also higher than usual, with 13,667 patients arriving at A&E.

Advertisement
Hide AdAdvertisement
Hide AdThere was also an increase in admissions from A&E. Last month 2,501 patients were admitted after turning up at A&E, a 16 per cent rise on 2017.
The unusually hot weather has been blamed in part for the rise, with many patients turning up with respiratory problems and dehydration.
The pattern was repeated across the country. Across England almost 2.2 million patients attended A&E in July, 100,000 more patients than the same month in 2017, with emergency admissions also rising by 6.3 per cent.
Gail Naylor, Nursing, Midwifery and Allied Health Professionals Director at Lancashire Teaching Hospitals NHS Foundation Trust, said: “It is widely appreciated that demand for NHS services has increased continuously in recent years.
Advertisement
Hide AdAdvertisement
Hide Ad“With many of us living longer, more and more people are developing complex or long-term conditions which require NHS services.
“That means we are increasingly looking after more acutely unwell patients in our hospitals all year round.
“Extreme weather do bring additional pressures on our services but our staff continue to work day-in, day-out, with great commitment and compassion .
“However, we do need the public’s help in making sure that our staff are able to concentrate on providing the care required by those most in need.
Advertisement
Hide AdAdvertisement
Hide Ad“Local pharmacists can provide a wide range of help and advise on how to treat a number of minor conditions. Likewise, the free NHS 111 helpline is available 24 hours a day, 7 days a week, for help on how to treat a minor injury or illness as well as advice on where to go for the most appropriate and timely care if you do need to see a health care professional.
“We are continuing to work with our partners on the ‘Our Health Our Care’ programme to consider, with the public’s input, how services in Central Lancashire should be provided in the future to address these demand challenges which our NHS services now face all year round. “
An NHS England spokesman said: “As temperatures soared, the NHS saw an unprecedented summer surge last month with a record 2.2 million patients attending A&E, and, thanks to the hard work of staff, nine in 10 people were seen, treated and admitted or discharged within four hours.”
In Lancashire, 85.2 per cent of people were seen, treated and admitted or discharged within the four hour target period.
Advertisement
Hide AdAdvertisement
Hide AdThat’s down on July 2017 when 88.8 per cent were dealt with in four hours. Hospitals are supposed to admit or discharge 95 per cent of patients within the target time.
Three years ago 94.9 per cent were seen within four hours.
Earlier this summer, the Post reported on predictions from the British Medical Association that the summer would see an unusually high level of demand.
National BMA chairman Dr Chaand Nagpaul said: “Doctors and patients have just endured one of the worst winters on record, resulting in thousands of cancelled operations, unacceptable long waits to be seen and people who are already at their most vulnerable having to face the indignity of being treated in hospital corridors.“These scenes have become an all-too-familiar annual occurrence.
“We cannot accept that this is the new normal for the NHS.”
Nick Scriven, president of the Society for Acute Medicine, said the increased admissions during the heatwave had given staff no respite from the pressures and stresses of winter.
Advertisement
Hide AdAdvertisement
Hide Ad“What is of particular concern now, however, is that the summer months are traditionally the time acute hospitals and frontline staff have to recharge the batteries - this year we have had no respite and draining conditions,” he explained.
“Last year NHS leaders admitted it took until October to recover from winter 2017 and we are now only a few months away from the next onslaught.”
Donna Kinnair, director of nursing policy and practice at the Royal College of Nursing, said: “With rising A&E attendance and admissions, hospitals up and down the country are now seeing winter conditions in summer, putting extra pressure on services that have barely recovered from the cold weather earlier this year.
“Nurses are seeing more cases of heart failure, renal failure and dehydration - all conditions linked to hotter weather.
Older people are particularly at risk. With 20 per cent more trusts breaching the four hour A&E target in July compared to June, it’s clear our understaffed services are struggling to cope.”